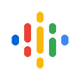
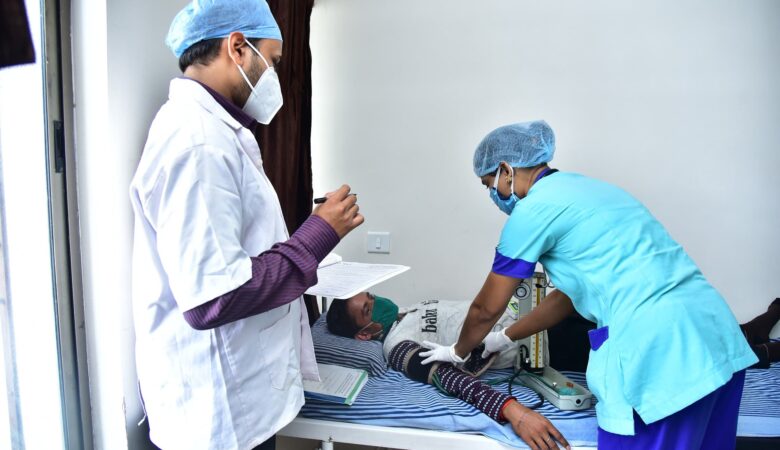
Peculiarities of medicine in different countries of the world
We’ve Helped The Following Brands

Get essay writing help in no time or complete your research on a health system effortlessly with our experienced writers. We always meet deadlines and requirements! Order 24/7.

Save on medicines and medical procedures with discount coupons from promocodius.co.uk. On our website you will always find current promotional codes of popular pharmacies and medical institutions in Britain

All USA airports by the state on Airportix.

List of online casinos offering birthday bonuses in Japan.

Who has called me? How do I know who it is and why they’re contacting me?
Alcoholism is the major cause of car accidents in Ontario. Make sure to check the drink and drive limits in Ontario before driving.

Don’t miss out on your chance to win big jackpot at 10-line-loto.com. With a simple sign-up, you’re steps away from potentially life-changing lottery games!
Recent Publications
September is National Suicide Prevention Awareness Month. Unfortunately, preliminary data for 2022 showed the highest number of annual deaths due to suicide ever recorded. After adjusting for population growth and age, the suicide rate...
Heart Attack Prevention Techniques: Caring for Your Body and Mind
Nolan2023-08-31You're likely familiar with the alarming rate of heart attacks. You may have even witnessed someone grappling with this...
Artificial intelligence in the modern US healthcare system
Nolan2023-03-24From day to day, more and more we hear about Artificial Intelligence and its implementation in different spheres, including...
The Importance of Rest for your Health: Why Taking Breaks is Essential
Nolan2023-03-17In today's fast-paced world, it's common to push ourselves beyond our limits and work long hours without taking proper...
Surprising Health Benefits Of Gambling That You Did Not Know
Nolan2023-01-04Many people have never thought gambling and health benefits could appear together in a statement. When one pictures a...
Rising Healthcare Infrastructures in Nigeria
Nolan2023-01-04Nigeria lacks modern healthcare infrastructure. Nigeria has among Africa's lowest healthcare indices. With 5.5 healthy births per woman and...
United States
Nolan2022-09-26The United States ranks at the bottom of the Commonwealth Fund's international comparison reports, despite the fact that America...